You’ve tried the medications, pushed through the physical therapy appointments, and maybe even explored a few procedures, yet the pain keeps coming back. For many adults living with chronic joint, spine, or musculoskeletal conditions in North Dallas, this cycle feels exhausting and discouraging. The reality is that lasting pain relief rarely comes from a single treatment. It comes from a structured, evidence-backed process that addresses root causes, accounts for your specific health profile, and scales interventions appropriately from least invasive to most advanced.
Table of Contents
- What you need before you begin
- Step 1: Activate nonpharmacologic therapies
- Step 2: Medication escalation and risk management
- Step 3: Interventional and regenerative options
- Putting it all together: Step-by-step summary
- What most chronic pain guides miss: Honest evidence, evolving strategies
- Connect with pain management experts for personalized care
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Non-drug therapies first | Exercise, physical therapy, and mind-body approaches should be your first steps for chronic pain relief. |
| Medications require caution | Escalate to medications only when truly needed, reassessing for risks and effectiveness. |
| Regenerative options vary | PRP and stem cell treatments can help some patients, but evidence is mixed and not guaranteed. |
| Personalized care matters | Work with providers to set goals and tailor a plan based on your condition, needs, and preferences. |
What you need before you begin
Before any treatment plan can succeed, you need a clear framework. Step-by-step chronic pain management in adults should start with setting goals such as reducing pain, maximizing function, and improving quality of life while prioritizing nonpharmacologic and complementary therapies alongside treatment of comorbid mental health conditions. This is not a minor detail. Skipping the goal-setting phase often leads to unfocused care and poor outcomes.
A thorough clinical assessment is equally essential before beginning treatment. Ruling out serious or progressive disease, such as fractures, tumors, or inflammatory conditions, ensures that your treatment plan is safe and appropriate. Conditions like SI joint pain are frequently misdiagnosed or treated without a proper baseline evaluation, which delays recovery significantly.
Mental health comorbidities deserve particular attention at this stage. Depression and anxiety are highly prevalent among people with chronic pain, and each condition can worsen the other in a reinforcing cycle. Identifying and treating these conditions early increases the likelihood that physical interventions will work as intended.
Key prerequisites before starting a pain management plan:
- Set concrete goals: reduce pain intensity, restore daily function, and improve overall quality of life
- Complete a thorough assessment to rule out serious pathology requiring urgent intervention
- Screen for depression, anxiety, and sleep disorders that can amplify pain perception
- Commit to a plan that favors holistic pain relief strategies as a foundation
| Assessment element | Why it matters | When to act |
|---|---|---|
| Diagnosis confirmation | Ensures appropriate treatment selection | Before any intervention |
| Mental health screening | Comorbidities reduce treatment efficacy | At initial evaluation |
| Functional baseline | Measures progress over time | Before and during care |
| Goals documentation | Guides shared decision-making | Before starting treatment |
With goals set and foundational health checked, you can confidently move into first-line pain management steps.
Step 1: Activate nonpharmacologic therapies
Evidence consistently points to nonpharmacologic therapies as the right starting point for most chronic pain conditions. A nondrug approach first is favored for chronic low back pain in most cases, rather than defaulting to medications at the outset. This guidance from the American College of Physicians has shifted how pain specialists approach first-line care, and for good reason.
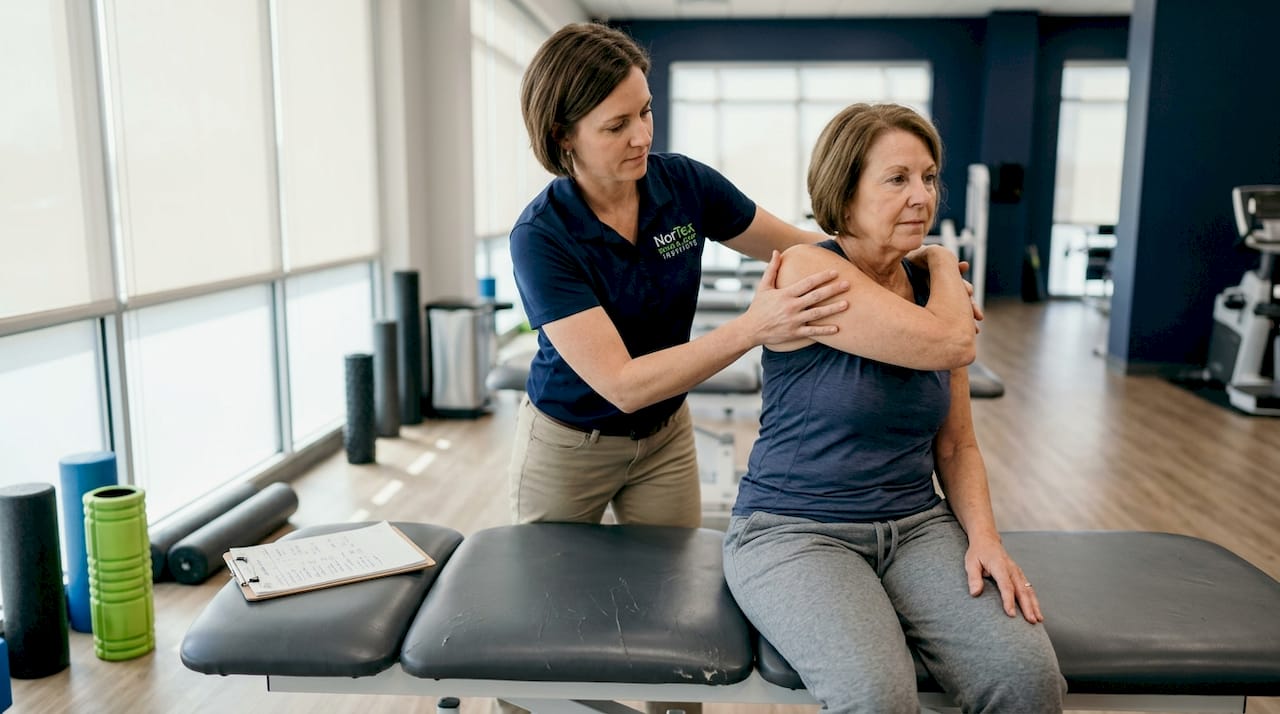
The evidence base for exercise and physical therapy is particularly strong. Movement-based interventions improve tissue mobility, reduce inflammation-related sensitization, and strengthen the supporting structures around painful joints and spinal segments. Structured programs tailored to your specific condition, whether that involves aquatic therapy, resistance training, or guided mobility work, tend to outperform generic exercise advice.
Nonpharmacologic modalities for chronic low back pain include exercise, physical therapy, cognitive behavioral therapy (CBT), and mindfulness-based stress reduction (MBSR), with acupuncture and spinal manipulation also considered depending on evidence quality. NSAIDs are recommended only when these approaches prove insufficient. This stepwise prioritization protects patients from unnecessary medication exposure and allows clinicians to observe how the nervous system responds to less invasive interventions.
Evidence-based first-line nonpharmacologic therapies to consider:
- Exercise and physical therapy: Prioritize condition-specific movement protocols under professional supervision to reduce pain and restore functional capacity.
- Cognitive behavioral therapy (CBT): Addresses pain-related thoughts, fear-avoidance behaviors, and psychological barriers to recovery that can sustain chronic pain cycles.
- Mindfulness-based stress reduction (MBSR): Structured mindfulness practice reduces central sensitization and improves pain tolerance through neurological pathways.
- Acupuncture: Moderate-quality evidence supports its use for chronic low back pain, neck pain, and osteoarthritis-related discomfort.
- Spinal manipulation: Relevant for select patients with mechanical low back or neck pain when performed by qualified practitioners.
- Tai chi and yoga: Demonstrated benefits for balance, flexibility, and pain reduction in older adults and those with joint conditions.
Pro Tip: Combining two or more nonpharmacologic strategies, such as physical therapy alongside a mind-body pain therapy program, often produces better results than either approach alone. The nervous system responds well to multi-channel input.
| Therapy | Evidence quality | Best suited for |
|---|---|---|
| Exercise/physical therapy | High | Most chronic musculoskeletal conditions |
| CBT | Moderate-high | Pain with psychological overlay |
| Acupuncture | Moderate | Low back, neck, osteoarthritis pain |
| MBSR | Moderate | Widespread or centralized pain syndromes |
| Spinal manipulation | Moderate | Mechanical spinal pain |
Understanding what options exist makes finding the best low back pain treatments much more manageable. Additionally, patients often find value in starting with home remedies for low back pain alongside supervised care. If these nonpharmacologic steps provide meaningful relief, further escalation may not be necessary.
Step 2: Medication escalation and risk management
When nonpharmacologic therapies alone do not achieve adequate pain control, a careful, stepwise approach to medication becomes appropriate. The goal is not to replace non-drug strategies but to augment them selectively. NSAIDs (nonsteroidal anti-inflammatory drugs) such as naproxen or ibuprofen are typically the first pharmacological option considered, offering both pain relief and anti-inflammatory benefits for musculoskeletal conditions.
If NSAIDs are insufficient or contraindicated, clinicians may consider alternatives like duloxetine (an SNRI with demonstrated efficacy for chronic pain) or tramadol (a weak opioid with a somewhat different risk profile than stronger opioids). These medications are used within a multimodal framework that keeps non-drug therapies active throughout. For short-term management of acute flares, SI joint steroid injections can also reduce inflammation directly at the source.
The evidence is clear: Stepwise opioid use principles emphasize minimizing risk through multimodal care and vigilant reassessment. Stronger opioids are reserved for situations where other options have genuinely failed or where potential benefits clearly outweigh the risks for that individual patient.
Opioids, when necessary, are not a standalone solution. They carry significant risks including dependence, cognitive impairment, and reduced efficacy over time due to tolerance. Responsible prescribing requires reassessment within one to four weeks of initiation or dose escalation, with ongoing monitoring of pain scores, functional status, and risk indicators.
Key principles for safe medication management in chronic pain:
- Use medications as one layer within a multimodal, integrative treatment plan
- Prefer NSAIDs or non-opioid alternatives before escalating to stronger agents
- Reassess frequently (within 1 to 4 weeks) after starting or changing any medication
- Combine pharmacologic care with non-drug strategies to reduce dependence risk
- Understand opioid step-down strategies and discuss an exit strategy with your provider from the start
- Explore pain management alternatives before assuming stronger medication is the only path forward
If medication escalation is not sufficient, or if you prefer to avoid prolonged pharmacological management, advanced interventional and regenerative options represent the next meaningful step.
Step 3: Interventional and regenerative options
Regenerative medicine has expanded the options available to patients who have not found adequate relief through conventional nonpharmacologic and pharmacologic approaches. Platelet-rich plasma (PRP) therapy, which involves concentrating platelets from your own blood and injecting them into damaged tissue, is among the most widely discussed regenerative treatments in musculoskeletal pain management.
For PRP specifically, evidence varies by condition, and one systematic review and meta-analysis in chronic noncancer pain reports PRP may reduce pain and can outperform corticosteroid or hyaluronic acid injections in certain scenarios, though the authors also describe the evidence base as limited and heterogeneous. This is an honest characterization of where the science currently stands, and patients deserve that transparency before committing to treatment.
Stem cell therapies represent another regenerative frontier. For knee osteoarthritis, stem cell injections may slightly improve pain and function, but with low certainty and ongoing uncertainty about long-term harms and structural effects. This does not mean these treatments lack value. It means they work best when applied to the right patients, for the right conditions, with realistic expectations clearly established upfront.
One significant source of variability in regenerative outcomes is preparation methodology. Heterogeneity in PRP preparation, including differences in platelet concentration, activation technique, and leukocyte content, can drive inconsistent outcomes across clinics and studies. Patients should ask specifically how PRP is prepared and what concentration protocols are used at any clinic they consider.
Pro Tip: Before choosing regenerative therapy, review condition-specific evidence. PRP for arthritis has more supporting data than PRP for certain spinal conditions, so the right conversation with your provider should be tailored to your exact diagnosis.
How to approach regenerative therapy responsibly:
- Confirm that nonpharmacologic and medication-based options have been adequately trialed first.
- Review condition-specific evidence, not just general claims about PRP or stem cells.
- Ask your provider about preparation protocols, expected timelines, and realistic outcomes.
- Understand that PRP therapy limitations are real and that some conditions respond better than others.
- Engage in shared decision-making that weighs your functional goals against the uncertainty in the current evidence base.
Reading further about common misconceptions around PRP and understanding PRP as an arthritis strategy will help you ask better questions and set appropriate expectations.
Putting it all together: Step-by-step summary
The chronic pain management process works best when each phase builds logically on the one before it. Skipping steps or jumping to advanced interventions prematurely often produces disappointing results and can delay finding an approach that genuinely works. The expert workflow follows a clear sequence: assess for serious disease, activate nonpharmacologic therapies, incorporate behavioral and mind-body strategies, add medications if needed, and consider interventional or regenerative options only after clear indications, realistic expectations, and shared decision-making are in place.
Complete step-by-step sequence:
- Assess: Rule out serious pathology, establish functional baseline, screen for mental health conditions.
- Set goals: Define what success looks like in terms of pain, function, and daily quality of life.
- Activate non-drug therapies: Begin exercise, physical therapy, and mind-body strategies as primary care.
- Add medications if needed: Start with NSAIDs, escalate selectively, reassess frequently.
- Consider interventional options: Nerve blocks, joint injections, or SI joint procedures for targeted relief.
- Evaluate regenerative therapies: PRP or stem cells for appropriate diagnoses with realistic expectations.
- Reassess continuously: Track pain levels, functional capacity, and quality of life at regular intervals.
| Step | Primary options | Evidence level | Practical note |
|---|---|---|---|
| 1. Assessment | Clinical evaluation, imaging | Foundational | Must precede all treatments |
| 2. Nonpharmacologic | Exercise, PT, CBT, acupuncture | High to moderate | First-line for most conditions |
| 3. Medications | NSAIDs, duloxetine, tramadol | Moderate | Use only after step 2 is tried |
| 4. Interventional | Injections, nerve blocks | Moderate | Targeted for specific diagnoses |
| 5. Regenerative | PRP, stem cell therapy | Low to moderate | Patient selection is critical |
Incorporating effective home remedies alongside clinical care also supports recovery between appointments, and understanding what makes PRP therapy effective helps patients evaluate whether it fits their specific situation.

What most chronic pain guides miss: Honest evidence, evolving strategies
Most articles about chronic pain management present a clean, linear process. The reality is messier, and acknowledging that is actually more helpful to patients than projecting false confidence. Pain management is deeply personal. Two patients with identical MRI findings can have vastly different pain experiences, functional limitations, and treatment responses. That variability is not a failure of medicine. It is a feature of how complex chronic pain truly is.
The same honest assessment applies to regenerative medicine. Platelet-rich therapies for musculoskeletal soft-tissue injuries are not one-size-fits-all solutions. Effects are condition-specific and depend heavily on preparation protocols and patient selection. Any clinic presenting PRP or stem cell therapy as a guaranteed solution without acknowledging evidence uncertainty is not giving you the full picture.
We also see a recurring problem with opioid management in chronic pain: patients are started on medications without a clear exit strategy or robust non-drug support in place. Opioid risk mitigation depends on reassessment and combining opioid therapy with non-opioid and nonpharmacologic strategies to reduce long-term dependence and adverse outcomes. That combination is not optional. It is the standard of care, and patients should expect it from their providers.
The most effective chronic pain care we see at Nortex Spine and Joint involves patients who stay engaged, ask hard questions about their treatment evidence, and commit to the non-drug strategies even when they feel less exciting than an injection or procedure. The patients who understand PRP honestly, set realistic goals, and participate actively in their own care consistently report better long-term outcomes than those who arrive expecting a single treatment to resolve years of accumulated pain.
Connect with pain management experts for personalized care
If you recognize yourself in this guide, whether you are still searching for the right starting point or wondering whether regenerative therapy might finally provide the relief you have been looking for, our team at Nortex Spine and Joint is here to help you build a plan that fits your specific situation. We offer a full spectrum of regenerative medicine solutions tailored to your diagnosis, history, and goals. From evidence-based PRP therapy for pain relief to customized rehabilitation and interventional procedures, our approach is always grounded in realistic expectations and honest evidence. Explore our full range of all pain management treatments and take the next step toward lasting relief.
Frequently asked questions
What are the first steps in chronic pain management?
Step-by-step management should begin with setting clear goals, ruling out serious conditions, and prioritizing nonpharmacologic therapies like exercise, physical therapy, and mind-body approaches. Assessment of comorbid mental health conditions is also an important early step.
When is it appropriate to use medications for chronic pain?
Medications are considered after nonpharmacologic therapies prove insufficient, starting with NSAIDs or non-opioid alternatives before escalating. Stepwise opioid principles reserve stronger options for cases where other treatments have genuinely failed, with reassessment required within one to four weeks.
How effective are regenerative treatments like PRP or stem cells?
Regenerative options show mixed evidence across musculoskeletal conditions, with some studies reporting modest improvements in pain and function. Results depend heavily on diagnosis, preparation protocols, and patient selection, making shared decision-making essential.
Are mind-body approaches supported by evidence for pain relief?
CBT and MBSR have moderate to high quality evidence supporting their use in chronic pain management, particularly for conditions with a significant psychological or central sensitization component. These approaches are recommended as first-line strategies, not last resorts.
Recommended
- Lower Back Pain Relief Tips That Really Work – Nortex | Pain Management | Allen, Garland, McKinney & Plano Texas
- Non-Opioid Pain Relief: Effective Options for Chronic Pain
- How to Relieve Lower Back Pain at Home: A Quick Guide for Fast Relief – Nortex | Pain Management | Allen, Garland, McKinney & Plano Texas
- Chronic Pain Relief with PRP Therapy: A Step-by-Step Guide – Nortex | Pain Management | Allen, Garland, McKinney & Plano Texas







